2025: Deadliest Ebola Strain Strikes DR Congo Again

2025: Ebola strikes DR Congo again. Kasai faces Zaire Ebola virus with 81 cases, 28 deaths, and urgent vaccination efforts underway.
The Negative Truth About Cholera in Africa
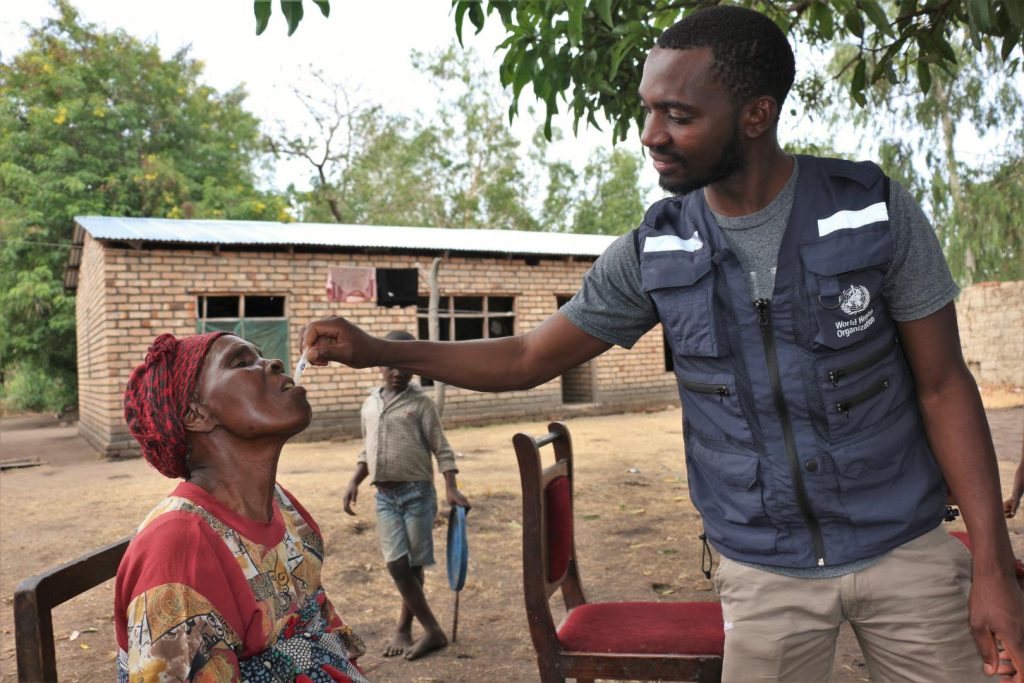
Explore the hidden truth about cholera in Africa—recent outbreaks, death tolls, and why strengthening rural health systems is critical to stopping the disease.
What About Rural Health? Convener Bags WHO Civil Society Appointment

‘What About Rural Health?’ Convener Appointed to WHO Civil Society Commission Steering Committee
When There Is No Pharmacist

Without a pharmacist, rural communities face deadly risks from unsafe drug use. Discover why pharmacists are vital for safe, effective care.
SO WHAT ABOUT RURAL HEALTH?

Explore rural health challenges and solutions—from access gaps to telemedicine—and why investing in rural care benefits us all.
Before the Next Outbreak: What the world must know

Recent viral outbreaks show rural communities are first hit—and least prepared. Here’s why strengthening rural healthcare is a global priority.
Gavi 2025: What a $9Bn Pledge Means for the World
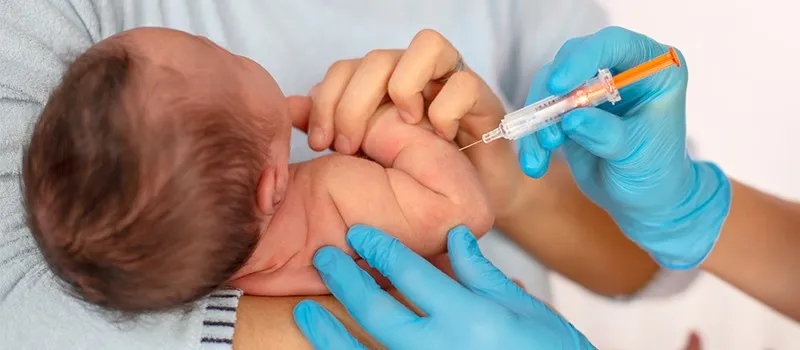
What does a $9B pledge mean for vaccines, health equity, and the future of global immunisation? Discover the key takeaways from the Gavi Summit.
Low Fertility Rate Is Not The Crisis — Inequality Is

A Women’s Reaction to the Real Global Fertility Rate Crisis By Chinasa Imo | What About Rural Health? Global Fertility Rate Is Falling — But That’s Not the Whole Story The global fertility rate is on the decline. According to the UNFPA’s 2025 State of World Population Report, the global average now sits at 2.2 births per woman—down from 5 in the 1960s. By 2050, it’s expected to fall below the replacement level of 2.1. But here’s the critical point: the crisis isn’t that people are choosing smaller families. It’s that millions are unable to have the number of children they want—because of poverty, healthcare gaps, and systemic inequality. The Real Crisis? Reproductive Agency UNFPA surveyed 14,000 people across 14 countries and found that: “1 in 4 people haven’t had or expect they won’t have their desired number of children.” It’s not biology that’s the problem—it’s barriers. 257 million women worldwide want to avoid pregnancy but lack access to modern contraception (UNFPA, 2025).This isn’t a personal shortcoming — it’s a systemic failure. That’s where the popular “fertility crisis” narrative falls apart. It assumes people are making free, empowered choices — but for many, that freedom doesn’t exist. Take Namrata, a working mother in Mumbai, whose story was featured by the BBC. She and her husband hoped for a second child, but the high costs of raising just one — from healthcare to school fees — made that feel out of reach. Her experience mirrors findings from the UNFPA survey, where the most common reasons for not having more children were: lack of money, lack of time, and lack of support. When policymakers say, “people are choosing to have fewer children,” we need to pause and ask: is it truly a choice? Because the data tells a different story: Many are having fewer children than they would like — not out of preference, but due to financial strain and structural barriers. Others are having more than they intended — because they lack access to contraception and control over their reproductive lives. In both cases, the common thread is a loss of agency. It’s not just about birth rates — it’s about whether people can actually decide for themselves. In Rural Communities, Fertility Rate has a Grim Face In remote areas of countries like Nigeria, India, and South Africa, women face compounding obstacles: Long distances to clinics High maternal and infant mortality rates Limited contraceptive options Child marriage and low educational opportunities And while urban discussions focus on fertility incentives and work-life balance, rural women are still fighting for access to basic healthcare. You can’t make empowered choices when you’re facing gender-based violence, malnutrition, forced marriage, and poverty every day. In such conditions, “choice” is an illusion. While sub-Saharan Africa hasn’t reached below-replacement fertility, early shifts are emerging due to urbanization, increased education, family planning access, and gender equality efforts—contributing to a gradual, organic decline. The takeaway? Behind every data point is a real story. And behind every fertility decline is a system.Instead of asking how many children women are having, we should be asking: why are they having fewer—or none at all? Stop Treating Women as Birthrate Solutions Countries like Hungary, South Korea, and China are now offering cash incentives and launching pro-natalist campaigns to boost birth rates. But this approach misses the mark. Rather than creating inclusive systems that respond to what women actually need, these governments are pressuring women into motherhood (Lee, 2025; Friedman, 2024; Kwon, 2024; Tan, 2023). Policies rooted in panic will always fall short.True reproductive justice means building systems of care that support informed, empowered choices—whether that’s having children, not having them, or choosing to wait. Fertility support should begin with rights, not rewards. More: Why Hungary’s Subsidies Failed Saying “No” Can Be a Powerful Act One of the most powerful insights from the UNFPA report is this: many women aren’t avoiding children because they don’t want them—it’s because the system makes it too risky. For some, choosing to stop at one or none isn’t apathy—it’s survival. As a woman in the Philippines put it: “A lot of policies are against women’s healthcare. It pushes us to stay single and have no children.” (UNFPA, 2025, p. 9) When systems fail—through violence, poverty, or inadequate care—women don’t give up. They opt out to protect themselves.This policy feedback loop is not apathy; it’s risk management. Reframe the Narrative: Fertility Should be About Choice Rather than crafting policies to manipulate fertility rates, we need to shift the focus to what truly matters: supporting women to thrive. When women—especially in rural communities—feel safe, heard, and supported, they make choices that benefit their families and society. The real issue isn’t low birth rates. It’s that too many women still lack the agency to make life-defining decisions about their bodies and futures. What’s needed are policies that trust women, invest in health systems, and create conditions where reproductive autonomy is not the exception—but the norm. At WhatAboutRuralHealth?™, we believe the solution isn’t more babies. It’s more support, options, and freedom. Rural women must be at the center of reproductive health conversations—not as passive recipients or population targets, but as leaders. They deserve dignity, care, and platforms to be heard. That means: More investment in rural health systems More protection from gender-based violence More clinics More spaces—like this one—for rural women to speak their truth Because the real fertility crisis isn’t about numbers. It’s about equity.True progress is when every woman can say:“Yes, I want a child.”“No, not right now.”“This is enough for me.” What You Can Do Reproductive justice = reproductive choice. If you’re a health worker, policy expert, or rural community member, we want your voice in this conversation. Submit your rural health story here Join our volunteer collective References UNFPA State of World Population Report 2025 BBC: The Real Fertility Crisis CBS News: Korea’s Parenthood Incentives Financial Times: Hungary’s Demographic Policies
Rural Health: This Campaign Is Urgent

by Elijah Nsikak In the heart of rural communities worldwide, a quiet crisis unfolds daily. From limited access to healthcare services to health disparities, underserved populations face unique challenges often overlooked in broader health discussions. As we launch our campaign, it’s imperative to highlight these issues and understand why immediate action is essential. The Rural Health Landscape: A Global Perspective Rural areas are home to approximately 46 million people in the United States alone, accounting for about 15% of the population . Globally, billions reside in rural settings, often with limited access to essential healthcare services. These communities frequently experience higher rates of chronic diseases, mental health issues, and maternal and infant mortality compared to their urban counterparts. Disparities in Healthcare Access One of the most pressing issues in rural health is the shortage of healthcare professionals. In the U.S., as of September 2024, 66.33% of Primary Care Health Professional Shortage Areas (HPSAs) were located in rural areas . India: In Maharashtra’s Jalgaon district, a woman was forced to deliver her baby on the roadside due to the unavailability of ambulance services . This incident highlights the dire state of rural healthcare infrastructure in parts of India. China: In rural China, David Wei had to carry his nephew on his back for 3 kilometers (1.9 miles) along a rough, under-construction road after the young man suffered a heart attack—while they waited 90 minutes for an ambulance to arrive from the city. Shortage of healthcare providers means that rural residents travel long distances for medical care, leading to delayed diagnoses and treatment. This barrier is exacerbated by limited transportation options and inadequate infrastructure. Socioeconomic Factors and Health Outcomes Disadvantaged communities often grapple with socioeconomic challenges that directly impact health outcomes. Higher poverty rates, lower educational attainment, and limited employment opportunities contribute to poorer health status among rural populations. These factors also influence lifestyle choices and access to health-promoting resources, leading to higher incidences of obesity, smoking, and physical inactivity. Consequently, residents of rustic areas are at an increased risk for conditions such as heart disease, diabetes, and many more health risks. The Impact of Hospital Closures Over the past decade, rural hospitals have been closing at an alarming rate. In the U.S., more than 130 rural hospitals have shut down since 2010, with financial constraints and low patient volumes cited as primary reasons . These closures not only limit access to emergency and specialized care but also have broader economic implications, including job losses and decreased community investment. The Role of Technology and Telehealth Telehealth has emerged as a potential solution to bridge the healthcare gap in rural areas. However, the effectiveness of telehealth is contingent on reliable internet access, which remains a significant hurdle. A KFF analysis found that nearly 3 million Americans live in areas lacking both healthcare and reliable high-speed internet, hindering telehealth services. The Urgency for Policy and Advocacy Addressing rural health disparities requires concerted efforts from policymakers, healthcare providers, and community organizations. Strategies include incentivizing healthcare professionals to practice in these areas, investing in infrastructure, and tailoring public health initiatives to meet the unique needs of rural populations. Moreover, incorporating the voices of residents in low-resourced communities policy development ensures that interventions are culturally appropriate and effectively address the specific challenges these communities face. Join the Movement Our campaign aims to spotlight the pressing issues in rural health and advocate for sustainable solutions. By raising awareness, sharing stories, and promoting evidence-based policies, we strive to create a more equitable healthcare landscape for all. We invite you to be part of this movement. Together, we can make a difference. Read about the $9Bn pledge for global health
AHA announces recipients of 2024 Rural Health Leadership Award

The AHA today announced the team from Columbia Memorial Hospital, a critical access hospital in Astoria, Ore., is the 2024 recipient of the Rural Hospital Leadership Team Award. The award recognizes rural hospital leaders who guide their hospitals and communities through change and innovation. Also recognized as finalists were teams at Atrium Health Lincoln in Lincoln, N.C.; Schneck Medical Center in Seymour, Ind.; and Summit Pacific Medical Center in Elma, Wash. The award will be presented at the 38th annual AHA Rural Health Care Leadership Conference, taking place Feb. 23-26 in San Antonio.
